Acute Bacterial Conjunctivitis: Clinical Approach and Treatment Guide
- Mayta

- 9 hours ago
- 3 min read
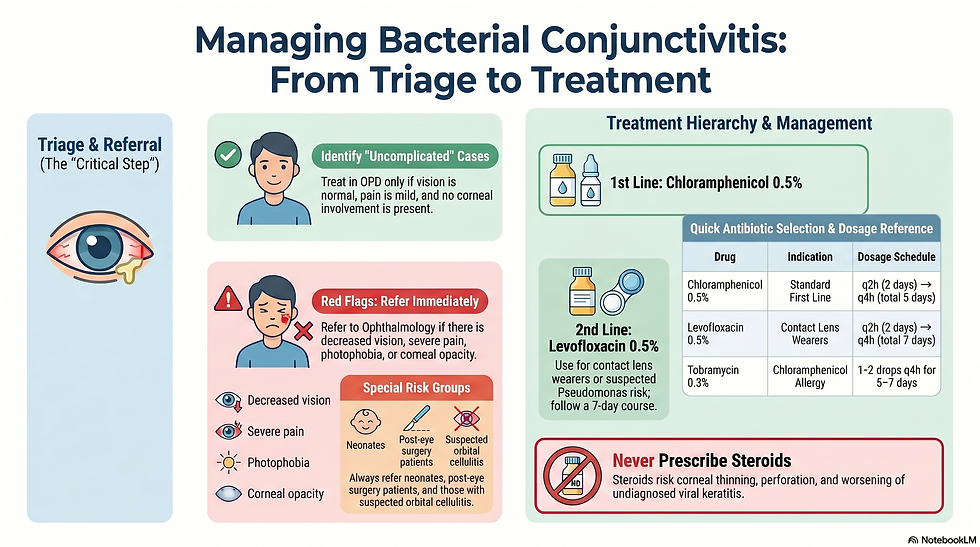
1. Clinical Definition
Acute bacterial conjunctivitis = superficial infection of the conjunctivaTypical features:
Red eye
Mucopurulent discharge (sticky eyelids in morning)
Mild irritation (NOT severe pain)
Usually normal vision
2. Determine Severity First (CRITICAL STEP)
Before prescribing anything, classify:
✅ Uncomplicated conjunctivitis (OPD case)
ALL must be present:
No vision loss
No severe pain
No photophobia
No corneal involvement
No contact lens–related keratitis suspicion
No recent eye surgery
No systemic severe disease
Not neonate
👉 This is the ONLY group you treat empirically in OPD
❌ Complicated / RED FLAG → REFER OPHTHALMOLOGY
If ANY present:
↓ Visual acuity
Moderate–severe eye pain
Photophobia
Corneal opacity / ulcer / keratitis
Contact lens wearer with red eye
Pseudomembrane
Severe unilateral red eye
Trauma / foreign body
Post eye surgery
Neonate
Suspected orbital/periorbital cellulitis
👉 These are NOT conjunctivitis until proven otherwise
3. Management Setting
👉 Uncomplicated → OPD
No admission needed.
4. Treatment Strategy (Evidence-based + Exam-oriented)
🔑 Key concept (AAO / NICE)
Many cases are self-limited (5–7 days)
Antibiotics = shorten duration slightly
No antibiotic is clearly superior
5. Drug Selection Hierarchy (VERY IMPORTANT)
🥇 FIRST-LINE (Standard answer)
Chloramphenicol 0.5% eye drops
Prescription:
Chloramphenicol (0.5%)1 drop, affected eye(s),q2h while awake × 2 days → then q4h,for 5 days total
Why is this the first line:
✅ Broad coverage (Gram + / Gram –) ✅ Cheap, accessible ✅ Low resistance in community use ✅ Guideline-supported (NICE primary care)
🥈 SECOND-LINE (Special situations)
Levofloxacin 0.5% (Fluoroquinolone)
Prescription:
Levofloxacin (0.5%)1–2 drops, affected eye(s),q2h while awake × 2 days → then q4h,for 7 days
Indications:
✅ Contact lens wearer ✅ Suspected Pseudomonas risk ✅ Concern for early keratitis ✅ Failure of first-line
Why NOT first-line:
❌ Overly broad ❌ Resistance concern ❌ Cost ❌ Stewardship principle
🥉 ALTERNATIVE OPTIONS
1. Tobramycin 0.3%
Prescription:
Tobramycin (0.3%)1–2 drops, affected eye(s),q4h, for 5–7 days
Used when:
Cannot use chloramphenicol
Alternative aminoglycoside coverage
2. Poly-Oph (Neomycin + Polymyxin B + Gramicidin)
Prescription:
Poly-Oph1–2 drops, affected eye(s),qid (1×4), for 5–7 days
⚠️ Important Clinical Concerns with Poly-Oph
❌ Why NOT first-line:
Neomycin → high allergy risk
Combination = unnecessary for mild disease
No added benefit vs single-agent therapy
When acceptable:
✅ Mild–moderate infection ✅ Cannot use chloramphenicol ✅ Need broader empirical coverage
When to avoid:
❌ History of drug allergy (especially neomycin)
❌ Suspected viral conjunctivitis
❌ Contact lens-related red eye
6. Supportive Treatment (MUST INCLUDE)
Even if antibiotics given:
Clean discharge (sterile saline / clean water)
Hand hygiene
Avoid touching eyes
Stop contact lens use
Warm compress if needed
7. What NOT to do (HIGH-YIELD)
❌ Steroid eye drops→ Risk of:
Worsening herpes keratitis
Corneal thinning → perforation
❌ Treat all red eyes as bacterial→ Viral is more common
❌ Use fluoroquinolone routinely→ Resistance + overkill
8. Follow-Up Plan
Expected improvement: 2–3 days
Full resolution: ~5–7 days
Re-evaluate if:
No improvement after 3–5 days
Symptoms worsen
New pain / photophobia / vision loss
👉 Then refer to ophthalmology
9. Quick Exam Summary
🧠 Core Answer:
Uncomplicated → OPD
1st line → Chloramphenicol
Contact lens → Levofloxacin
Alternative → Tobramycin / Poly-Oph
🔑 Ultimate Clinical Logic
👉 “Most cases are mild → use simple drug”
👉 “Only escalate when risk increases”
🎯 Final Clinical Ordering Template
Diagnosis: Uncomplicated bacterial conjunctivitis
Setting: OPD
Definitive treatment:
Chloramphenicol (0.5%) 1 drop q2h → q4h × 5 days
Supportive treatment:
Eye hygiene, warm compress, stop contact lens
Education:
Avoid contamination
Return if worse
Follow-up:
3–5 days or earlier if red flag



Comments